Lancet Neurol:缺血性卒中患者预防性使用肝素治疗并未获益
2013-05-28 Lancet Neurol dxy
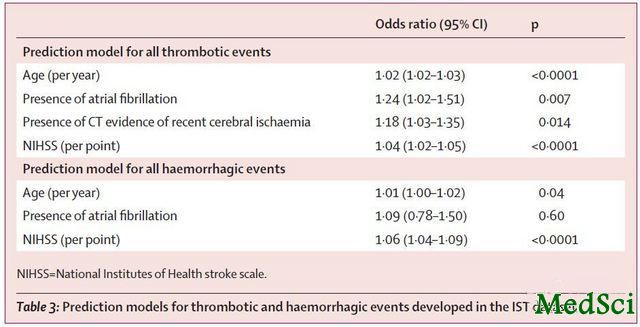
血栓栓塞性事件及出血性事件的预测模型 一直以来,有高凝状态的卒中患者推荐使用肝素预防血栓栓塞性事件。很多国际卒中治疗也推荐,对于静脉血栓形成高危或低出血风险的卒中患者使用肝素预防血栓形成。但治疗效果尚不明确,来自英国的William N Whiteley 等医师汇总了卒中治疗方面的几项大型临床试验,其目的是确定选择抗凝治疗的可靠方法,从而降低卒中死亡率及重度残疾状态。研究结果发表在2013年5月
一直以来,有高凝状态的卒中患者推荐使用肝素预防血栓栓塞性事件。很多国际卒中治疗也推荐,对于静脉血栓形成高危或低出血风险的卒中患者使用肝素预防血栓形成。但治疗效果尚不明确,来自英国的William N Whiteley 等医师汇总了卒中治疗方面的几项大型临床试验,其目的是确定选择抗凝治疗的可靠方法,从而降低卒中死亡率及重度残疾状态。研究结果发表在2013年5月的Lancet neurology杂志上,结果显示:当缺血性卒中患者血栓栓塞事件的风险较高或出血事件风险较低时使用肝素治疗并未获益。
该研究的数据来源于五项大型缺血性卒中的随机对照试验,这些试验均包含肝素(普通肝素、肝素类似物或低分子量肝素)与阿司匹林或安慰剂对比治疗。根据研究特点制定卒中后14天内血栓栓塞事件(心肌梗死、卒中、深静脉血栓或肺栓塞)与出血事件(症状性颅内出血或明细的颅外出血)的统计预测模型。
高年龄卒中患者,神经功能损害严重;有心房颤动病史的患者,卒中后血栓栓塞事件及出血事件的风险均增加。除此以外,CT显而易见缺血性卒中证据的患者发生血栓栓塞事件风险增加。在此评估模型中,受试者工作特征曲线下面积预测血栓栓塞事件为0.63(95% CI 0·59—0·67),预测出血事件为0·60 (0·55—0·64)。该研究未发现当出现增加血栓栓塞事件风险或降低出血事件风险时增加肝素使用的有益证据。
研究结果显示,当缺血性卒中患者血栓栓塞事件的风险较高或出血事件风险较低时使用肝素治疗并未获益。因此从这些研究数据也无法确定选择早期抗凝治疗患者的方法。我们推荐适当修改卒中治疗中常规或选择性使用肝素的规定。
Targeted use of heparin, heparinoids, or low-molecular-weight heparin to improve outcome after acute ischaemic stroke: an individual patient data meta-analysis of randomised controlled trials.
BACKGROUND
Many international guidelines on the prevention of venous thromboembolism recommend targeting heparin treatment at patients with stroke who have a high risk of venous thrombotic events or a low risk of haemorrhagic events. We sought to identify reliable methods to target anticoagulant treatment and so improve the chance of avoiding death or dependence after stroke.
METHODS
We obtained individual patient data from the five largest randomised controlled trials in acute ischaemic stroke that compared heparins (unfractionated heparin, heparinoids, or low-molecular-weight heparin) with aspirin or placebo. We developed and evaluated statistical models for the prediction of thrombotic events (myocardial infarction, stroke, deep vein thrombosis, or pulmonary embolism) and haemorrhagic events (symptomatic intracranial or significant extracranial) in the first 14 days after stroke. We calculated the absolute risk difference for the outcome "dead or dependent" in patients grouped by quartiles of predicted risk of thrombotic and haemorrhagic events with random effect meta-analysis.
FINDINGS
Patients with ischaemic stroke who were of advanced age, had increased neurological impairment, or had atrial fibrillation had a high risk of both thrombotic and haemorrhagic events after stroke. Additionally, patients with CT-visible evidence of recent cerebral ischaemia were at increased risk of thrombotic events. In evaluation datasets, the area under a receiver operating curve for prediction models for thrombotic events was 0·63 (95% CI 0·59-0·67) and for haemorrhagic events was 0·60 (0·55-0·64). We found no evidence that the net benefit from heparins increased with either increasing risk of thrombotic events or decreasing risk of haemorrhagic events.
INTERPRETATION
There was no evidence that patients with ischaemic stroke who were at higher risk of thrombotic events or lower risk of haemorrhagic events benefited from heparins. We were therefore unable to define a targeted approach to select the patients who would benefit from treatment with early anticoagulant therapy. We recommend that guidelines for routine or selective use of heparin in stroke should be revised.
作者:Lancet Neurol
版权声明:
本网站所有注明“来源:梅斯医学”或“来源:MedSci原创”的文字、图片和音视频资料,版权均属于梅斯医学所有。非经授权,任何媒体、网站或个人不得转载,授权转载时须注明“来源:梅斯医学”。其它来源的文章系转载文章,本网所有转载文章系出于传递更多信息之目的,转载内容不代表本站立场。不希望被转载的媒体或个人可与我们联系,我们将立即进行删除处理。
在此留言







#Neurol#
45
#肝素治疗#
33
#缺血性卒#
34
#缺血性#
32
#Lancet#
33